Dental implants
Implantology in Laval
When a tooth is non-restorable, it is necessary to extract it. There are quite a few situations that may lead to this such as: extensive decay, coronal or root fracture, a considerable periapical abscess, a periodontal abscess, considerable tooth mobility, etc.
In most cases, the tooth then requires a replacement of some sort because the dental arch becomes asymmetric and less resistant to the forces of mastication. Adjacent teeth may drift and loss bone support. The ability to masticate properly diminishes as well. Loss of anterior teeth becomes a cosmetic issue.

The old traditional method of replacing teeth is with a removable partial denture that hooks onto the remaining dentition. One can only imagine how unstable this may be. Another method would be a bridge, which is cemented onto the neighbouring teeth. Patients prefer this option, but it can only be used to restore spaces missing up to 2 or 3 teeth because otherwise the occlusal forces become too important to withstand.
The revolutionary method to replace teeth is by placing titanium screws into the jawbones, which serve as anchors for the future prosthesis. In the 1950s, Swedish dentist Dr Branemark discovered that titanium is the most biocompatible metal for living bone and osseointegration occurs. Thus began the era of implantology.
A dental implant is a titanium screw that is place in the jawbones to serve as an anchor for the future restoration, its purpose to replace the root of the missing tooth. The supra-gingival portion of the tooth is replaced with a crown, which will be supported by the implant. Evidently, a longer and a wider implant with be able to withstand greater occlusal forces and thus confers a better prognosis.
Implant placement requires specific circumstances and may not be done in every case. One condition is sufficient bone volume. After a tooth is extracted, vertical and horizontal bone loss of up to 40-50% occurs. In fact, it’s the root that maintains bone height. The teeth’s roots are anchored in the jaws and offer a stable base to teeth. When a tooth is extracted, the roots no longer stimulate bone in this area during mastication, and the bone begins to deteriorate. When a patient loses all of their teeth, this considerably accelerates bone resorption in both the upper (maxilla) and lower (mandible) jaws.
Sometimes, bone must be added through a bone graft. A better result is obtained if the graft is placed at the moment of extraction. This allows socket (and bone) conservation.

In order to replace one or many missing lower teeth where there’s not a possibility of doing a bridge, we use removable partial dentures (RPDs). We call these cases “distal extensions”. These distal extension RPDs are not tooth borne and are only supported by gums and underlying bone of the edentulous ridge. They will lack stability and also contribute to bone resorption. Poor retention and inadequate mastication are often associated to this type of RPD. They are often uncomfortable because they are massive, as well as unstable during mastication and elocution (speaking). Bone resorption is even more considerable when we’re talking about a complete denture due to the increased pressure on the gums and mucosa and their underlying bone. With this being said, implants are the best solution to this and the best way to restore the edentulous ridge.
Limited bone has already been discussed as a contra-indication. Other contra-indications to dental implants may include high blood sugar, immune problems, poor oral hygiene, high cholesterol, and smoking.
In order to properly evaluate whether dental implants are right for you, a 3D scan, also known as a CBCT is necessary. Prior to the implant surgery, models of your jaws and a surgical guide are made. From a physiological point of view, implants are the best solution because not only does this biocompatible material provide a firm anchorage in your jawbones, but it also prevents future resorption of your alveolar ridge.
Dental implants
Replacing a tooth
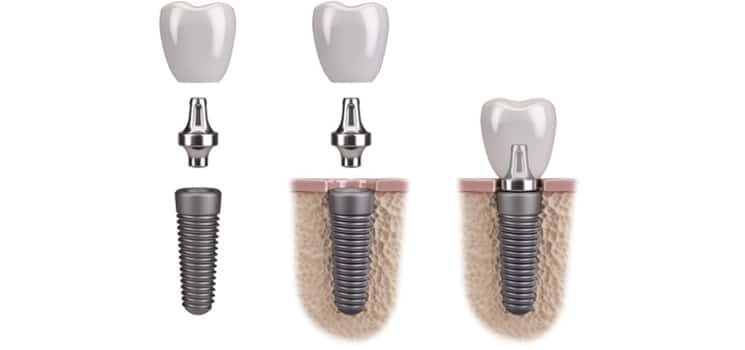
After a tooth is extracted, both vertical and horizontal bone loss can be observed. In order to place an implant, it is imperative that the implant be long enough and wide enough. To do so requires good bone quality.
Sometimes, bone must be added through a bone graft. A better result is obtained if the graft is placed at the moment of extraction. This allows socket (and bone) conservation.
It’s impossible to replace the last tooth on the arch, or multiple posterior teeth with a bridge, and long-term RPD use can lead to significant bone loss and unstable partials. In order to re-establish comfort and function, an implant-supported prosthesis may be proposed, after a proper clinical evaluation.
Limited bone has already been discussed as a contra-indication. Other contra-indications to dental implants may include high blood sugar, immune problems, poor oral hygiene, high cholesterol, and smoking.
If you have uncomfortable dentures, or multiple missing teeth that you wish to replace, we encourage you to make an appointment for a consultation. We will be able to answer your questions to the best of our ability and propose you a treatment plan that caters to your needs.
Dental implants
Did you know?

A endodontically-treated tooth with a crown on it has a good short- to medium-term prognosis (2-5 years), and a guarded long-term prognosis. An implant-supported crown has a very good long-term prognosis (10+ years).
Contact
Contact us today to book your next appointment and meet our experts.

